Hair Loss
Hair Loss – Alopecia
Hair loss, medically referred to as alopecia, is a common complaint among patients visiting the dermatologist and can be the source of significant physical and psychological stress. It is important to review some basic facts about alopecia in order to better understand the work-up and treatment options available for the type of hair loss you may be suffering from.
What is Alopecia?
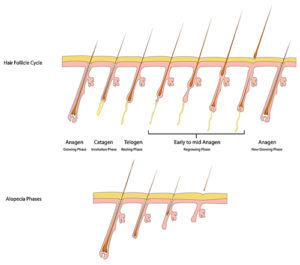
Hair grows in three phases: anagen (growth phase), catagen (regression phase), and telogen (resting phase). At any given time, about 83-85% of hairs are in anagen, 1-2% are in catagen, and about 10-15% are in telogen. The hair on the scalp is pre-programmed to shed approximately 100 hairs per day and to grow about 1cm/month. The number of times per week that you wash or brush your hair does not affect this growth and shedding cycle.
At the most basic level, alopecia can be categorized as either scarring or non-scarring. The difference between these two entities is that scarring alopecia causes damage to the hair follicle, which often results in irreversible hair loss. In non-scarring alopecia, follicular integrity is maintained and there may be potential for regrowth. Luckily, the non-scarring forms of alopecia are far more prevalent overall.
How to Slow Down or Reverse the Process of Hair Loss
If you feel you are suffering from increased shedding and/or thinning, there are several important things you can do at home and in conjunction with your primary care physician that may help stop, slow, or reverse the hair loss process.
1. If your hair loss or shedding is widespread, particularly if it is abrupt, you may be suffering from a condition called telogen effluvium. This is a period of increased shedding that usually occurs in the weeks to months following stress on the body. Common causes include pregnancy, new diets, some medications, recent illness or hospitalization, and emotional stress or trauma. This type of hair loss is reversible in almost all cases and your scalp density will return to normal usually within about 1 year. Check your medications (both over the counter and prescription) and discuss them with your primary care physician to see if any may be contributing to your hair loss. Never stop any prescription medication without first consulting with a physician.
2. If you cannot readily identify any of the potential causes of your new onset shedding or thinning, particularly if you are feeling more tired, your primary care doctor may want to run some common blood tests to assess your thyroid function, your iron stores, your red blood cell count, and your vitamin D level. If one or more of these are abnormal, oral medications can be given to fix the deficiency and your hair may return to its baseline. Before you see your doctor, consider supplementation with Vitamin D if you get very little sun exposure. In women, if hair loss is related to irregular periods or hair growth in unusual areas such as chin or lower abdomen, blood tests are recommended to identify if there is an underlying hormonal abnormality.
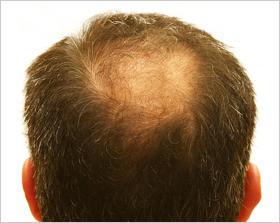
3. If your lab studies are normal, you may be suffering from the most common type of non-scarring alopecia, androgenetic (or male/female pattern) alopecia (AGA). This condition can affect both men and women and can start as early as adolescence. Despite many myths regarding the inheritance pattern, AGA can be passed down from any family member or it can present in a patient with absolutely no family history. AGA typically presents in a classic pattern with an increased loss at the temples and crown for men and an increased loss of the frontal scalp for women.
Male/Female Pattern Alopecia Treatments include:
- Minoxidil foam (Rogaine) over the counter
- Prescription Finasteride for men (Propecia)
- Supplements including Viviscal and Nutrafol
- Laser/Light devices to wear at home (by Hairmax, Theradome and Capillus)
- PRP (Platelet Rich Plasma Injections) – the most exciting new development to come along in years and now offered by Krauss Dermatology
4. If you or your child has coin-shaped or discrete patches of hair loss, the diagnosis may be a condition known as alopecia areata. This is a type of auto-immune related non-scarring hair loss that should be evaluated by a dermatologist. Treatment options are available and range from topical creams or solutions to cortisone injections to oral medications in more extreme cases. Spontaneous remission may also occur. For more information visit: www.naaf.org.
When Should I see a Dermatologist?
Warning signs that should prompt you to make a dermatology appointment include:
- Rapid onset and progression of hair loss with visible patches of bald scalp.
- Areas in the scalp where the hair has fallen out and the hair follicles can no longer be seen or appear scarred.
- Loss of hair in other parts of your body in addition to your scalp including your brows, lashes, and/or body hair.
- Increased itching, pain, scale or redness in the areas of hair loss.
These signs may indicate that you are potentially suffering from a scarring type of alopecia. While the scarring alopecias are generally uncommon, the emotional and psychological impact can be very distressing. The main goal for treatment of all scarring alopecias is to quell disease activity while preserving any remaining healthy hair follicles. Treatment options span from topical and systemic medications to more involved discussions about maximizing camouflage techniques. Please see the list provided at the bottom of this page for some recommendations for brow enhancement/ restoration and hair pieces (also called cranial prostheses). There are a multitude of resources and support groups available at The Cicatricial Alopecia Research Foundation. If you suspect you have scarring alopecia, make an appointment with a dermatologist.
Although insurance companies readily cover the cost of evaluation of scarring hair loss and alopecia areata, they often refuse to cover the most common types of hair loss. Unfortunately the cost of consultation and treatment is then the responsibility of the patient. If the suggestions we have discussed in this post and evaluation by your primary care doctor have not succeeded in improving your alopecia, your dermatologist can help investigate the cause of your hair loss and will create an individualized treatment plan that best suits you and your lifestyle. Hair loss, no matter what the magnitude, can be life-altering. At Krauss Dermatology, we will work with you to help minimize its impact.
Resource List
Brow and Lash Restoration
Prettyology
18 Newbury Street, 5th floor
Boston, MA 02116
(617)-262-1607
Website: www.prettyology.com
Contact person: Julie Michaud
Brow Enhancement Product
Wunderbrow
www.softsurroundings.com
Hair Replacement / Cranial Prosthesis
The Salon at 10 Newbury
10 Newbury Street
Boston, MA 02116
(617)-247-4900
website: www.salonat10newbury.com
Contact person: Patricia Wrixon
PK Walsh
75 Second Avenue
Needham, MA 02630
(781)-444-4414
website: www.pkwalsh.com
Patricia and Company Cosmetic Solutions
534 Main Street, #4
Weymouth, MA 02190
(781)-335-4700
website: www.patriciaandcompany.com
Contact person: Patricia Queeny

